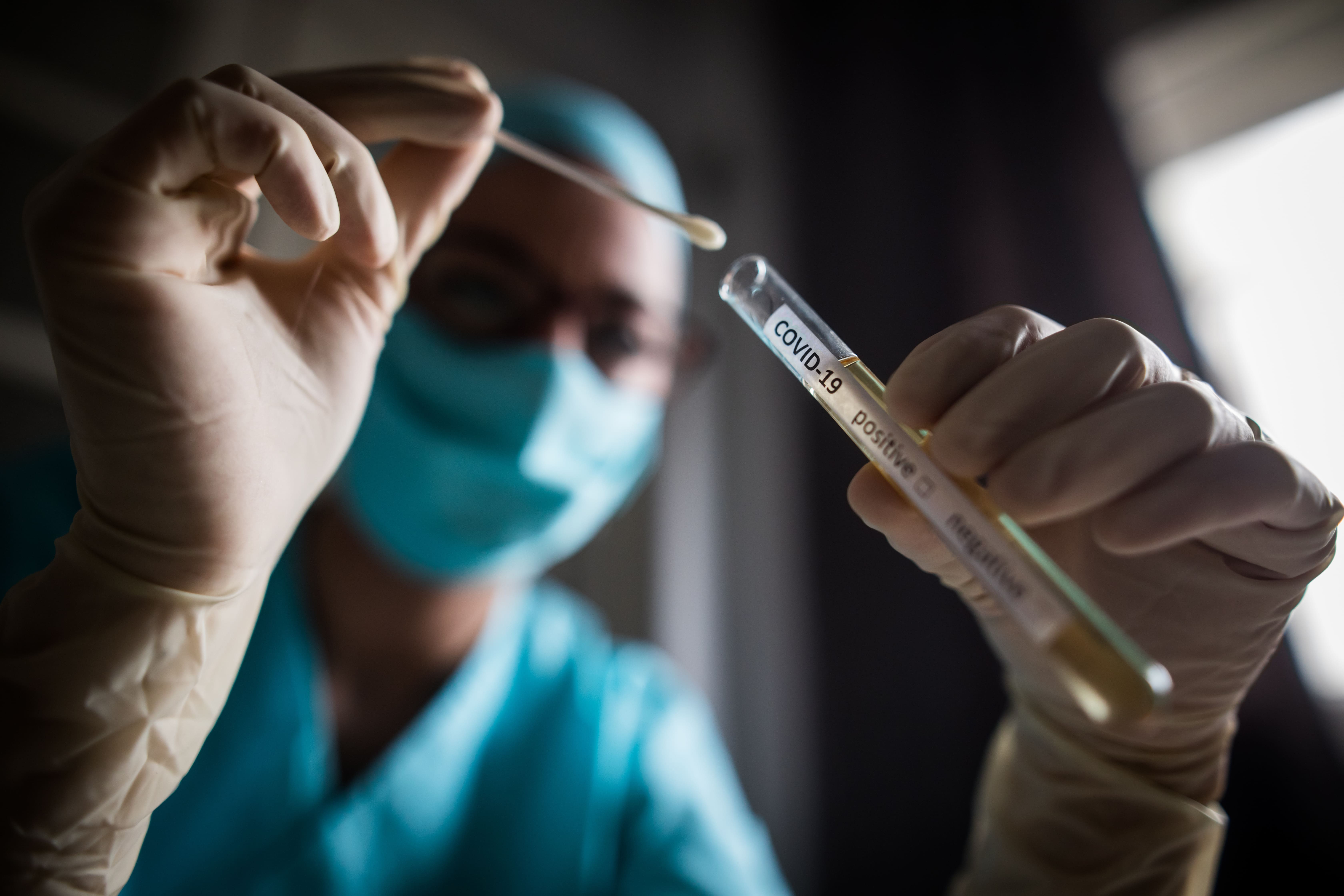
Bridging the gap between general practice and specialist care
It’s estimated that 0.4-1.3% of the Australian population identifies as trans and gender diverse - up to 338,000 people. A suite of transgender pathways is having a direct impact on how GPs support trans and gender diverse people.
Key insights
- Improved GP capability – Clinicians are better equipped to support trans and gender diverse people with clearer guidance and contemporary best practice.
- Stronger primary–specialist linkages – Pathways reduce gaps between general practice and specialist care, improving navigation and referral for patients.
- Wider system adoption – Multiple health systems have adopted the pathways, increasing consistency and access to up to date transgender health information.
- Faster access to specialist care – Education and pathway use have reduced waiting times for specialist appointments from around 300 days to about 30.
GP visit the first step
For many trans and gender diverse people, a visit to their GP is a first step towards asking for support or medical intervention. But with few GPs trained in transgender health, the experience can be variable.
When a GP in Hunter New England, New South Wales contacted the local HealthPathways team requesting tools to support gender diverse patients, adult endocrinologist and Conjoint Professor at the University of Newcastle, Katie Wynne was also seeing more and more transgender patients. She saw a need to build capacity more widely.
‘I had 1 trans patient and then 3 and then 10 and so I was on a steep learning curve for trans health. One of my first patients was actually a professor and we ended up writing a book on transgender health together,’ she says.
HealthPathways seemed like an appropriate way to really bridge the gap between general practice and specialist care in the hospital.
- Katie Wynne, Adult Endocrinologist and Conjoint Professor, University of Newcastle
Taking up the challenge
The Hunter New England HealthPathways team took up the challenge and became the first HealthPathways team in New South Wales to develop transgender pathways.
The process started with a working group back in 2016. Clinical Editor Sandra Fitzgerald remembers it clearly. ‘We have a rigorous process in Hunter New England when we’re starting a pathway. We get the key clinicians in the room and ask what’s working and what isn’t. It's usually primary and tertiary care providers but this was unique for us - this was the first time we directly involved community members in writing a pathway.’
Katie Wynne adds ‘At that point it was incredibly hard to access any gender-related healthcare, so it was really insightful. We're one of the first systems to use an informed consent model, so for adults, moving away from quite a gatekeeper approach to trans health, to really centring the person in the forefront of it. I think that that really helped us evolve our pathway so that it was incredibly contemporary for its time.’
The GPs in the room for that initial working group had not had a lot of experience with transgender health. Sandra says, ‘They weren't experts and so they could really look through the lens of a GP seeing a trans patient for the first time and were able to provide insights into what support was needed and how the pathway could best support that consultation.’
Dynamic area of medicine
Hunter New England is the lead region for NSW for the suite of three transgender pathways. Of the remaining 12 NSW/ACT HealthPathways programmes, 9 have become attached followers of some or all of the suite. This suite receives an average of 15 to 20 views per day across NSW/ACT since the lead region pathways went live.
Sandra says the success of the pathways is largely due to the efforts the HealthPathways team and specialists like Katie have put into promotion and education. ‘We've done a number of educational events. We regularly present at conferences. Most recently we have held a number of workshops on estradiol implant insertion and showcased the gender affirming hormone pathway.’
The pathways are constantly updated - often within a few weeks of new recommendations being released.
It's such a dynamic area of medicine. HealthPathways is really the only tool that has the power to update and distribute new information so regularly.
- Katie Wynne, Adult Endocrinologist and Conjoint Professor, University of Newcastle
Taking note at a state level
Now, the Ministry of Health is taking note at a state level. ‘The Ministry is interested in having more engagement with HealthPathways around trans health and resource mapping - because we are really on the front foot when it comes to resource mapping,’ says Katie.
Of course, the real impact of the pathway is on the people seeking support. And this is where Katie feels most pleased. ‘I’m really proud of how we’ve been able to build capacity. We published a paper showing that just an hour of education for health workers using HealthPathways was able to increase the capacity of clinicians to facilitate trans healthcare. We’ve been able to reduce the time to see a specialist by tenfold - from 300 days down to around 30.’
Want to explore how HealthPathways can support your health system? Get in touch.