Experiences from an Australian regional primary health network using HealthPathways as an enabler of a learning health system.
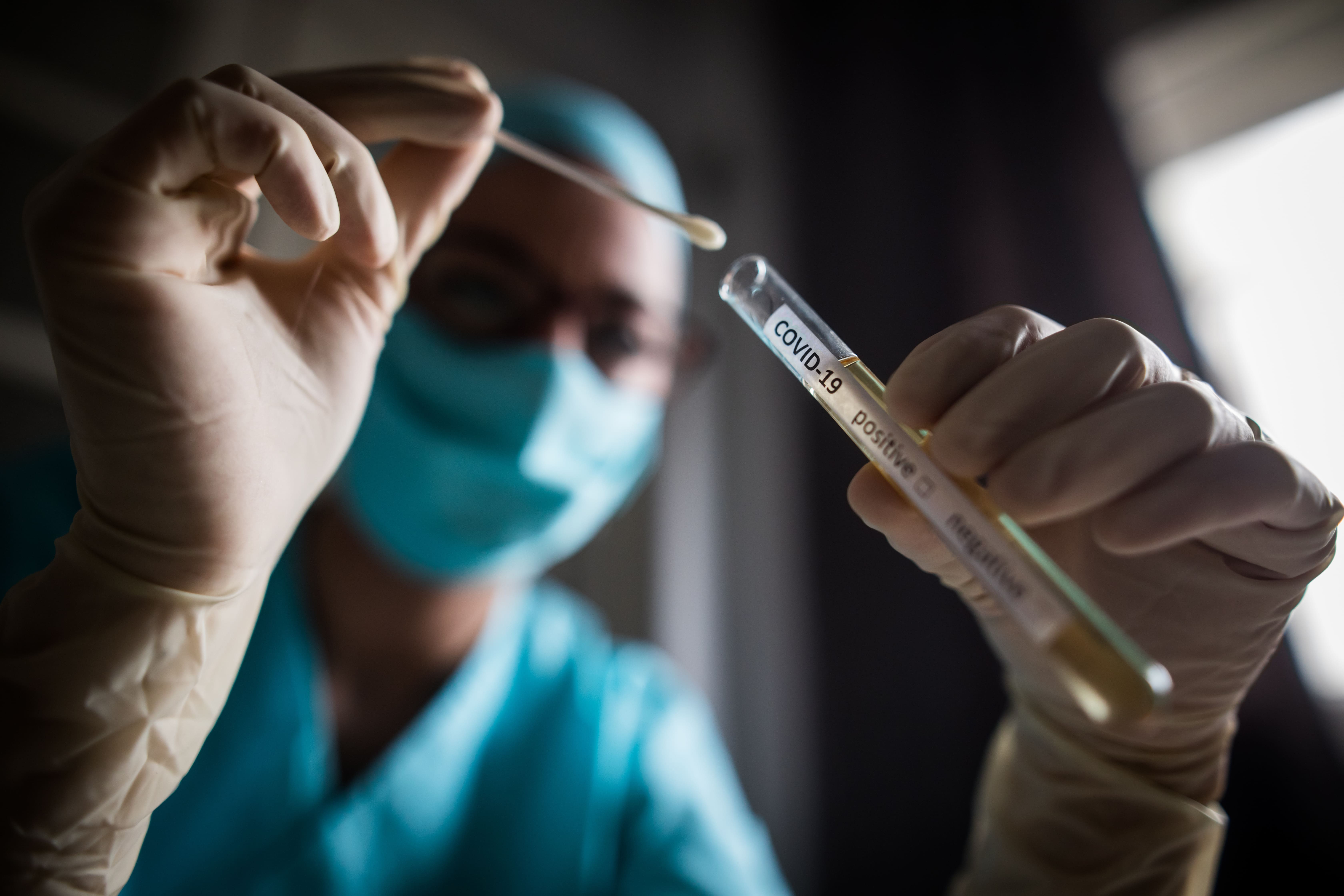
The COVID-19 pandemic challenged primary care to rapidly innovate. In response, the Western Victoria Primary Health Network (WVPHN) developed a COVID-19 online Community of Practice (CoP) comprising healthcare practitioners, administrators, and consumers. This 2024 report describes the transformation from crisis to self-sustaining learning health system.
Key insights:
- Collaboration drives better outcomes - Bringing clinicians together led to faster problem-solving and improved care coordination during the pandemic.
- Learning systems improve performance - Embedding a learning health system approach helped the region achieve leading results in COVID vaccination rates and GP antiviral prescribing.
- Shared knowledge builds resilience - Regular knowledge exchange and co-developed care models strengthened the PHN’s ability to respond to future health challenges.
- Theory-informed change sustains progress - Using established frameworks ensured that improvements weren’t just short-term fixes but became part of ongoing practice.
From crisis mode to continuous learning
Western Victoria Primary Health Network (WVPHN) used the pressure of COVID-19 to build something more durable than a rapid response – they built a regional, primary careled learning health system (LHS).
Anchoredin Project ECHO and guided by the Menear LHS framework and Kotter’s change model, the team turned weekly Community of Practice sessions into a structured engine for knowledge to practice - and then made it stick beyond the pandemic.
What they built - and why it worked
At speed, WVPHN connected GPs, nurses, pharmacists, aged care and disability workers, public health experts, specialists, administrators, and consumers in a virtual Community of Practice, embracing the Project ECHO ‘all teach, all learn’ ethos to translate fast moving policy and evidence into local care. The sessions followed an intentional cadence - identify priority issues, gather and curate the best available data, align on practical guidance, and codify the outputs for the frontline.
The approach married LHS principles (data → knowledge → implementation) with eight disciplined steps for change, creating momentum and shared purpose across alarge rural catchment.
Results that mattered
Over the course of the pandemic, WVPHN created a space where learning could happen in real time and be rapidly translated into practice. Through regular forums, webinars and shared resources, clinicians and system leaders came together to make sense of change, adapt to emerging challenges, and apply knowledge directly in care settings.
What mattered most wasn’t volume, but momentum. Knowledge was being used where care happened, and the network becamea trusted mechanism for turning uncertainty into action. Alongside this, WVPHN supported the co-design of new models of care and pathways that helped under pin Victoria’s strong response to COVID-19, including vaccination and antiviral delivery.
Making learning visible (and reusable)
The work went beyond conversation. Each session fed into reflection, shared problem-solving, and practical outputs - from short-form learning resources to formalised clinical guidance. Insights we recaptured, refined, and embedded into HealthPathways, ensuring that learning was not lost but translated into tools clinicians could rely on.
A dedicated operational team helped scale what worked, turning the network into a testing ground for approaches that could be rapidly adopted across services.
From urgency to endurance
As the acute phase passed, the focus shifted from rapid response to sustainability. Governance was strengthened, learning processes were formalised, and the approach was broadened beyond COVID-19. What emerged was a durable model for continuous improvement - one that blended structured learning, reflection, and practical application.
The result is a replicable way of embedding learning into everyday practice, offering a blueprint for regions looking to strengthen system capability beyond crisis response.
The full story
The published report details the four development phases, the frameworks used, and concrete outputs - including participation metrics, governance steps, and examples of new pathways. This offers a clear blueprint for building a primary care LHS from the ground up.
Want to explore how HealthPathways can support your health system? Get in touch.