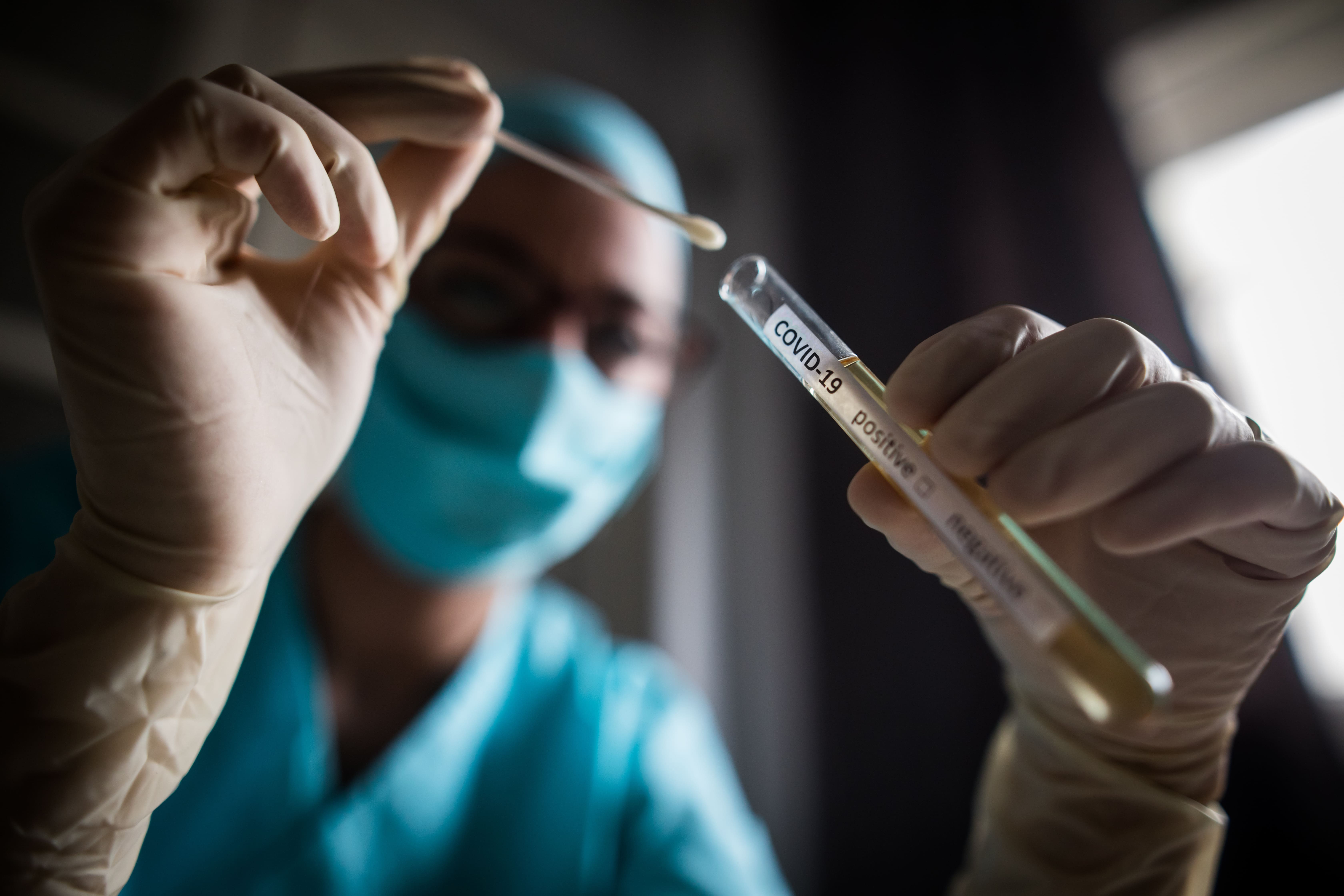
The value and impact of HealthPathways in the COVID-19 response
This 2023 report examines how HealthPathways strengthened the primary care response in New Zealand and New South Wales during COVID‑19. It highlights findings on improved clinician confidence, consistent care, system alignment, and effective feedback loops between frontline practice and policy.
Key insights:
- Improved clinician confidence and decision-making - GPs increasingly relied on HealthPathways as their primary source for COVID 19 guidance.
- Decreasing clinical variation and increasing equity - HealthPathways promoted consistent messaging and locally adapted protocols across regions.
- Increased trust across the health system - Collaborative pathway development built deeper relationships, bridging front-line feedback into policy refinement.
- Enhanced responsiveness through real-time feedback - Integrated feedback loops gave policy makers immediate insights, enabling rapid and iterative updates to guidance during the crisis.
Getting COVID‑19 policy into practice
This 2023 mixed‑methods case study by leading expert services and consulting firm Sapere examines how HealthPathways supported New Zealand and New South Wales to translate rapidly changing COVID‑19 policy and evidence into safe, consistent primary care during an exceptionally volatile period.
The study found HealthPathways provided a ‘one‑stop shop’ of reliable, locally relevant guidance that clinicians trusted at the point of care, enabling quick, safe decisions as advice and service configurations shifted day by day.
What they looked at - and why
The Sapere team reviewed programme maturity and usage across regions before the pandemic, analysed HealthPathways usage data (COVID‑19 and non‑COVID indicator pages), and interviewed stake holders including health‑system leaders, clinical editors, and programme teams. This approach allowed the case study to connect frontline experience with observable patterns in access and use, and to compare regions at different stages of implementation.
What changed during the response
HealthPathways became the practical mechanism for turning national and state guidance into local action. As public health settings and clinical recommendations evolved, pathways were updated rapidly and coupled with service‑specific details - testing access, referral routes, and escalation criteria - so clinicians could apply the latest best practice within local constraints.
Usage of COVID‑19 pages in HealthPathways rose in step with case waves. Non‑COVID indicator pages also increased in most regions, signalling broader uptake and reliance on HealthPathways through the crisis.
Why it mattered for the system
The work of developing and maintaining COVID‑19 pathways strengthened relationships, trust, and respect across government, local health services, colleges, and community providers.
HealthPathways also provided a direct feedback loop from frontline clinicians to policy‑makers via pathways and webinars, improving the clarity and feasibility of policy as the situation evolved.
The report concludes that HealthPathways reduced unwarranted variation while still enabling necessary local variation to support equitable outcomes - an important balance when services and risks differed by place.
The problem is GPs were getting information from so many sources. So we needed to sieve it and present in a simple and easy way for the frontline.
- HealthPathways clinical editor, New Zealand.
Signals that persisted
Beyond immediate response, the study reports sustained increases in HealthPathways usage after the initial waves, suggesting a step‑change in awareness and habitual use. For regions with more mature programmes pre‑COVID, higher baseline usage was evident; newer regions accelerated quickly under pressure, benefiting from established processes and shared assets.
Want to explore how HealthPathways can support your health system? Get in touch.